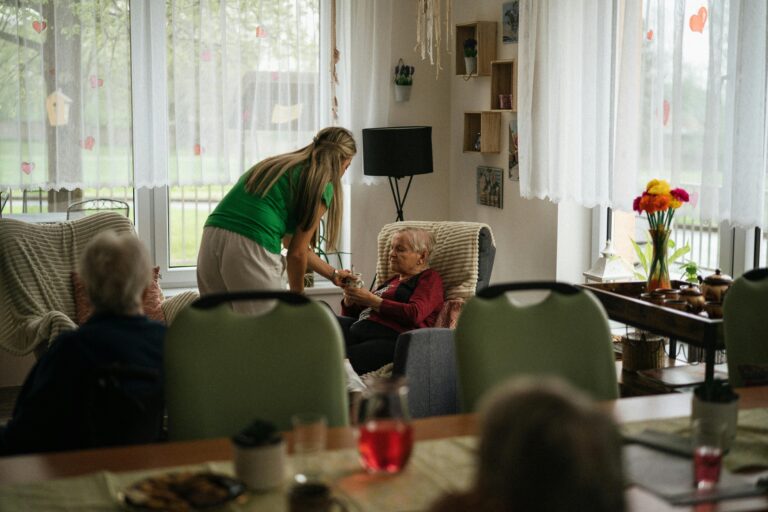
Protect Your Parents’ Savings From Nursing Home Expenses
Without proper planning, the high costs of nursing home care can quickly deplete your parents’ savings, leaving them financially vulnerable.
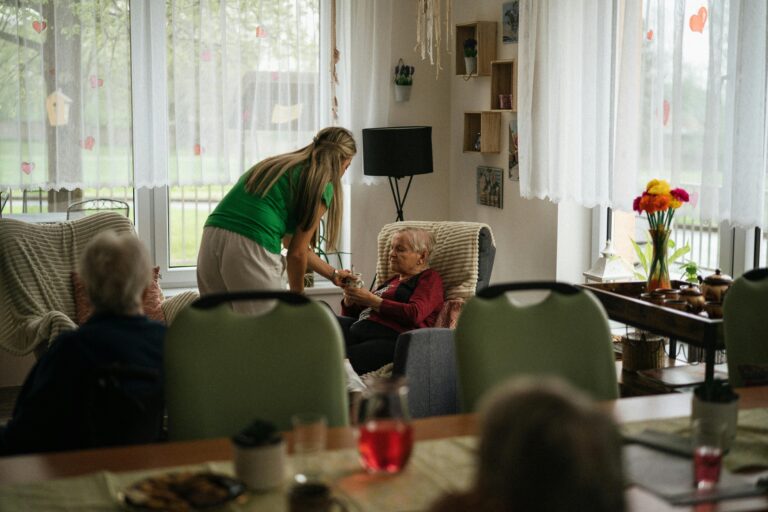
Without proper planning, the high costs of nursing home care can quickly deplete your parents’ savings, leaving them financially vulnerable.

Long-term care insurance helps cover costs of in-home care, assisted living and nursing homes. This protects your savings and secures your quality of life in your final years.

Navigating the myriad of ways to pay for nursing home care can be overwhelming. However, with a clear understanding of nursing home costs and the options available, it becomes manageable. Understanding Nursing Home Costs Nursing home costs nationwide can be daunting. In 2021, a semi-private room in a nursing home averaged $$7,908 per month, with private rooms at $9,034. Even assisted living facilities, which offer a lesser level of care than nursing homes, can run upwards of $4,500 a month. Most people who enter nursing homes start by paying for their care out-of-pocket by using their savings or accessing equity…

Retirement is when everything changes. Seniors may end up with new schedules, new hobbies, and even new homes. In the midst of all these exciting changes, don’t overlook the mundane: your insurance coverage.

Reaching the point where you need to consider residential options for your mother can be overwhelming. Not only is it emotionally fraught, there are also financial and legal considerations.

While the unpredictability of the future makes it difficult to plan ahead, becoming familiar with the options is important.

Discussing estate planning with your parents is a conversation that can be difficult to have. You might not want to think about the day they are no longer here, or even consider that they might experience a decline in health that severely limits their ability to think clearly or communicate with you.

Here’s what you need to consider, when looking to hire an elder law attorney.

Who needs long-term care insurance … and who might be able to do without it?

Elder Law is made up of three major categories, which can be broken down further into deeper topics.