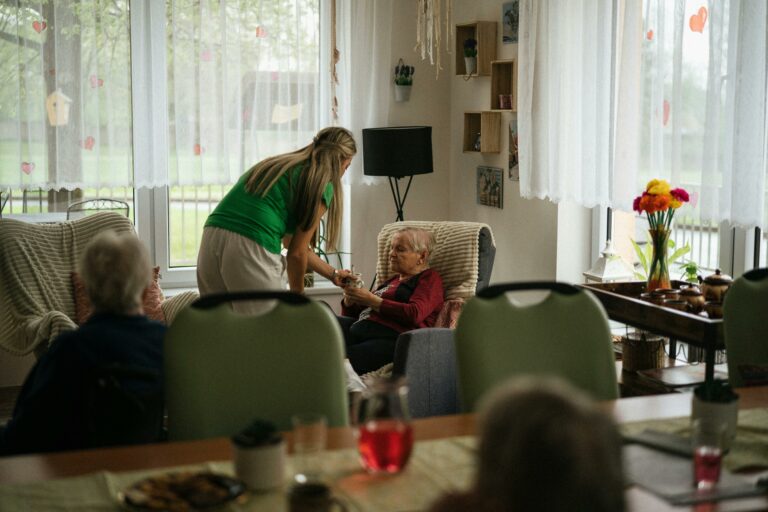
Caregiving and Estate Planning Provides Peace of Mind for All Generations
With so many responsibilities on a farming or ranching operation, caregiving plans can often get overlooked until it’s too late.
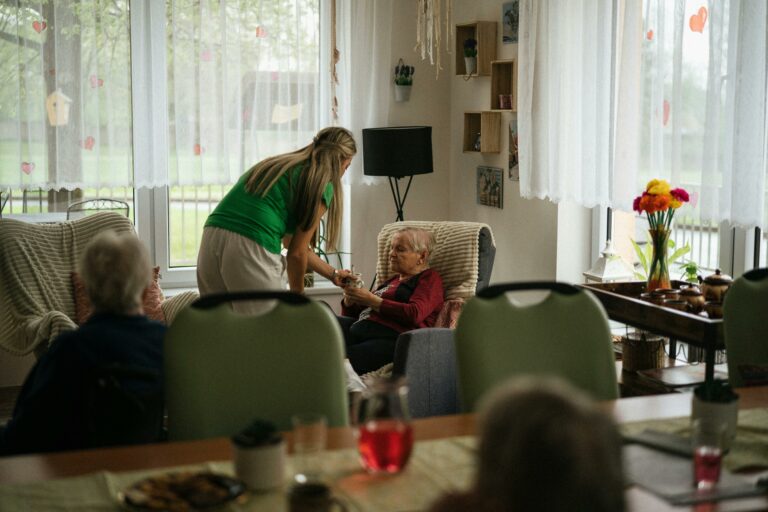
With so many responsibilities on a farming or ranching operation, caregiving plans can often get overlooked until it’s too late.

Depending on their medical condition, persons with dementia are often capable of making their own decisions regarding legal aspects, such as advance care planning.

Here are five ways to get started on this important issue of an aging parent’s finances.

An elderly man in Hernando County is back safe and sound with his family after being found through a tracking device planted by his wife.

Many people like to travel for rest, relaxation and inspiration — but there may be significant cognitive benefits as well.

An 87-year-old woman stranded for hours by a taxi company was given a free ride home in a fire engine, thanks to San Diego firefighters who noticed she was in distress.

Ever heard the phrase, “a chain is only as strong as its weakest link?” The same goes for a financial portfolio: It’s only as safe as the password that protects it.

As they get older, many — even most — Americans prefer to remain in their own homes as long as they can, AKA “age in place.” However, to do that, many will need to make their residences safer and easier to navigate, by making home modifications.

If caregiving looms in your future — and it likely does if you’re a daughter, an only child or the one (if you are, you know what I mean) — take time now to protect your financial life.

Once you have a list of promising agencies, arrange a consultation. AARP has a checklist of important questions to ask before signing a home health contract.